
Ophthalmology
Compiled by Dr. Khyne U Mar, DVM and Willem Schaftenaar, DVM
Eye problems are common in elephants. They are often the result of trauma and present as superficial or deep cornea lesions and ulcers. Cataracts are also regularly seen in elephants. If the vision in one eye is reduced, the animal should be approached with care from that side.
In a study in 1478 captive elephants (2956 eyes) in Thailand, 17.83% of the examined eyes from 369 elephants (24.97% of the total number of elephants) had anterior ocular abnormalities. The most common lesions in these examined eyes were frothy ocular discharge (5.85%), corneal edema (5.31%), and conjunctivitis (5.18%). In addition, epiphora, phthisis bulbi, other corneal abnormalities, anterior uveitis, and lens abnormalities were noted. Almost all lesions increased in frequency with age (Kraiwong, 2015). Regular ophthalmic examination in elephants should be included in their
annual health check program. Early detection and treatment of any ocular abnormality
may avoid the development of subsequent irreversible ocular pathology.
Clinical examination overview and diagnostic techniques
The clinical examination of the eye starts with the anamnesis (history) and observation of the animal.
The eyelashes should be long in order to protect dirt and objects from touching the surface of the eye. They are located mostly superior to the eye and can be as long as 11 cm. The inferior eyelid has less and smaller (2 cm) lashes.
A unique feature of the elephant eye is the lack of a lacrimal apparatus (lacrimal glands as well as nasolacrimal duct) and eye brows. Tear films simply flow towards the medial canthus and exit along a groove in the skin onto the face in Asian elephants (Wong et al. 2012).The area around the eyes is therefore often wet.
A Schirmer tear test can be performed in elephants. In a research cohort of 80 healthy Asian elephants the mean value was 34.3+/- 1.7 mm/min with older elephants (>40 years) having higher values than younger ones (<20 years).
The cornea should be clear, without any irregularities.
The iris of an elephant varies in color from tan, yellow, brown or the combinations.
Blepharospasm is a strong indication for ocular disease.
Conjunctiva cultures can be taken, though the strong palpebrae can make sampling for culture a challenge.
Ophthalmic anesthetics can be used safely in elephants and may facilitate clinical examination and allow ophthalmoscopic examination of the deeper ocular structures.
The pupillary light response can be performed if the elephant trusts the clinician enough to approach the animal with a proper light source at the required short distance. This test should be performed in subdued light.
The menace response can be performed if the animal allows the clinician at short distance by moving fingers towards the elephant's eye without causing air movement.

The numerous hairs on the skin of the palpebrae are not true cilia or true eyelashes as they are not associated with the margins of the palpebrae (Wong et al 2012, J. Zoo and Wildlife Med., 43(4), pp 793-801). The lower eyelid is more developed and ascends to a greater degree than the upper lid descends (Suedmeyer, 2006). (Photo KUMar)


The iris of an elephant can have several colors: tan, yellow, brown or a combination. (Photo: W.Schaftenaar)

A white, circumferential ring, similar to the arcus senilis in man is noticed in 40+ yr Asian elephant (fat deposit or aging?). (Photo: KUMar)
Fluorescein staining of the cornea may be difficult as the elephant will close its eye immediately when approached. A fluorescein strip can be placed in a 10 ml syringe with sterile water or saline; this solution can then be sprayed over the eye in a constant flow using a blunt small gauge needle. This should be sprayed on the eye from the medial or lateral side. It helps when at the same time a steady water stream is directed at the periocular skin, which may result in relaxation of the animal.
After fluorescein has been sprayed on the cornea, the eye should be flushed with sterile saline to remove excessive fluorescin. If present, cornea defects will stain green under blacklight and even under regular light.
Cataracts which appear as a white central spot and keratitis (diffuse, superficial cloudiness of cornea) are frequently seen in elephants. Vision can be checked by passing the light of a flashlight (or cell phone) from the ear over the eye to observe for a blinking reflex.
Ophthalmoscopy in the untrained elephant can be quite a challenge, as the animal will usually not allow this kind of close examination that moreover uses a light source. However, the animal can be trained to allow ophthalmoscopy.
The third eyelid or nictitating membrane is located at the ventro-medial aspect
of the orbit. Inside the nictitating membrane, an oblong, flanged-shaped piece of hyaline cartilage supports the anterior palpebral aspect of the nictitating
membrane. The harderian gland that is located here, plays a role in the lubrication of the cornea. Zeis's glands (modified sebaceous glands) are located in the margins of the lid. They produce an oily substance that helps lubricate the cornea.
The nictitating membrane in an Asian elephant (arrow).(Photo: KUMar)

Blinking reflex using a smartphone's flash light in an Asian elephant with chronic keratitis. (Video: W.Schaftenaar)
Ultrasonographic examination
The clinical examination of the elephant's eye can benefit from transcutaneous ultrasonographic examination. The anterior eye chamber, the lens end the posterior eye chamber can be visualized using a 4-7 MHz convex probe (Bapodra et al. 2010).
Following are descriptions of the anatomical components of the eye and the medical condition that may occur
Eyelids
Blepharitis is an inflammation of the eyelids than can be caused by trauma (rubbing), parasite infection or as part of a localized dermatitis. The accompanying symptoms are blepharospasm, epiphora (tearing that appears as wet skin area below the eye) and often photophobia. Sometimes lice (Haematomyzus elephantis) or ticks (Amblyomma tholloni) can be found on the eyelids causing local skin lesions.
Blepharitis in an Asian elephant. (Photo: KUMar)

Small skin lesion caused by ticks (Amblyomma tholloni)
(Photo: KUMar)


Conjunctiva
The conjunctiva is the tissue that lines the inside of the eyelids and covers the sclera (the white part of the eye). It is composed of unkeratinized, stratified squamous epithelium with goblet cells, and stratified columnar epithelium. The conjunctiva is highly vascularized, with many microvessels.
Conjunctivitis is an inflammation of the conjunctiva and is a common finding in elephants. In some cases small nodules and vesicles may be observed (lymphoid tissue on histology), possibly associated with chronic irritation. A conjunctivitis is often the result of trauma (hard object, dust, irritating liquid or smoke). Conjunctivitis is also seen in poxvirus infections.

Conjunctivitis in an Asian elephant (From: Elephant care manual for mahouts and camp managers, FAO 2005,
Conjuctivitis and keratitis in an Asian elephant. Note the swollen mucosa. (Photo: KUMar)

The conjunctival sac is a connection between the palpebral and bulbar conjunctiva. Under certain conditions (hypoproteinemia, trauma, insect bites or allergic reactions), a prolapse of this part of the cornea can develop, which protrudes like a mucosal sac between the eye and the lower eyelid.

Prolapse of the conjuncitival sac in an Asian elephant.
(Photo: KUMar)
Cornea
The cornea is transparent because it lacks cells and blood vessels and has no pigment. The cornea should always be wet thanks to a pre-corneal film tear. Oxygen and nutrients are available from the aqueous cornea tear film, the limbal capillary plexus and the palpebral conjunctival capillaries.
Several disorders of the elephant cornea have been reported. Most of the corneal lesions seem to have a traumatic cause: trauma by rubbing, allergy by environmental irritants such as exposure to direct sunlight or continued exposure to dryness or small particles, e.g. dust, smoke, grass seed etc. that damage the corneal epithelium.
Hypovitaminosis-A has also been suggested as a cause of cornea disorder as well as hypoproteinemia.
Acanthamoebae Spp. has been identified in corneal swabs. It's presence has been associated with corneal ulcers (Dangolla, 2005). However, the protozoa was also found in swabs taken from healthy elephant eyes (Wijesekara, 2007).
Corneal edema
Corneal edema, also called corneal swelling, is a buildup of fluid in the cornea. It is caused by dysfunction of the endothelial membrane on the inner side of the cornea, that normally pumps fluid out of the cornea in order to keep it transparent and clear. This can happen after a blow to the eye or a puncture of the cornea (e.g. by small branches), or by contact with toxic substances.
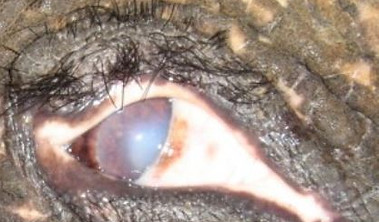

Cornea edema in an Asian elephant. (Photo: KUMar)
Cornea edema in an Asian elephant. (Photo: KUMar)
Cornea opacities - keratitis
Opacities in the cornea are called keratitis and are very common in elephants. They present as whitish, "cloudy" areas usually in the central part of the cornea. It has been suggested that they are caused by trauma (thorns, heat, dust, and chemicals), direct sunlight or chronic dehydration. The cornea must be checked for foreign bodies. In severe keratitis, the entire cornea turns white. This reduces the vision of the animal to only being able to distinguish just between light and dark. This can be tested with the blinking reflex. In some cases, keratitis can be painful: the elephant shows blepharospasm and the third eyelid may be protruded (partly) over the eyeball. In that case involvement of the iris should be considered.
It is recommended to perform cytology, aerobic bacterial culture, and sometimes fungal culture.
When opacities are only found in the superficial epithelium, and dispersed over the entire cornea surface, it might be the result of hypovitaminosis-A (vitamin A is essential for the normal functioning of the corneal epithelium, including the production of the tear film). This condition is called "xerophthalmia".
As fluid makes its way into the cornea it can accumulate and cause the
formation of small bullae or "blisters." This is called bullous keratopathy. If the
blisters break or rupture, a corneal ulcer will result.

Mild, superficial opacity in the central area of the cornea in an Asian elephant (keratitis). (Photo: KUMar)

Diffuse, superficial opacities spread over the entire cornea of an Asian elephant, possibly caused by hypovitaminosis-A (xerophthalmia). (Photo: KUMar)

Mild keratitis in an Asian elephant. (Photo: KUMar)
Severe keratitis involving the entire cornea of an Asian elephant. (Photo: KUMar)


Severe keratitis with protrusion of the third eyelid in an Asian elephant. This could be an expression of pain, in which case iris involvement should be considered. (Photo: KUMar)
Corneal ulcer
A cornea ulcer is an open sore on the cornea. The epithelial outer layer and the middle layer of the cornea (stroma) are disrupted. This condition is also called a melting corneal ulcer. Usually the primary cause is trauma of the cornea. This traumatic lesion can become infected by bacteria (Pseudomonas, Neisseria spp, fungi and other microbes. This condition is very painful and blepharospasm is often seen. The elephant may be rubbing the area around the affected eye against an object. There may be protrusion of the third eyelid.
An ulcer is usually the result of trauma. Treatment of keratitis with NSAID's or glucocorticosteroids increases the risk of ulceration.
As a reaction to the ulcer and to repair the lesion, blood vessels will grow into the stroma of the cornea, visible as small red lines, sometimes forming a network of small vessels. This process takes several weeks. When the cornea surface has been repaired, the remnants of these blood vessels will be visible as white connective tissue strands. The major risk in an ulcerated cornea is perforation of the entire cornea, which will result in loss of the ocular fluids and complete loss of the eye.
When blood vessels fail to grow towards the ulcer, the ulcer remains in an unchanged form as an indolent corneal ulcer, needing a special treatment.

Two manifestations of a severe keratitis and cornea ulcer with a prolapse of the iris in an Asian elephant. (Photo: KUMar)

Hypopyon
Hypopyon keratitis is an accumulation of pus (heterophils and fibrin) in the anterior eye chamber (between cornea and lens). It is accompanied by profuse discharge and signs of ocular pain. Ultrasonographic examination may be helpful for diagnosing pus in the anterior chamber. One case report describes the treatment of hypopyon in an Asian bull elephant. Hypopyon and uveitis have been described in a case of leptospirosis (Fowler. 2006. Infectious diseases. In: Fowler and Mikota, 2006, 403).
Iris and uvea
The iris is a diaphragm that regulates the influx of light. It is a very vulnerable structure that consists of two layers: the outer (anterior) pigmented fibrovascular layer (known as stroma, which lacks an epithelial layer) and the inner (posterior) surface covered by a heavily pigmented epithelial layer that is two cells thick (the iris pigment epithelium). This anterior surface projects as the dilator muscles. The high pigment content of the iris blocks light from passing through to the retina, restricting it to the pupil. The outer edge of the iris, known as the root, is attached to the sclera and the anterior ciliary body. The iris and ciliary body together are known as the anterior uvea.
Any lesions in the anterior part of the eye can result in damage to the iris. Parts of the affected iris may come into contact with the inner layer of the cornea (anterior synechia) or the lens (posterior synechia). If there is also a corneal ulcer, the iris may prolapse through the ulcer (iris prolapse). Iris lesions are considered to be very painful in all animal species. These conditions need immediate veterinary attention.
Lesions of the iris and uvea are called uveitis. If only the anterior part is involved, we call it iritis. In reality it will be hard to distinguish these conditions in elephant ophthalmology, unless proper ophthalmoscopy can be performed under sedation or general anesthesia.

Lens
The lens is a transparent biconvex structure in the eyes that, along with the cornea, helps to refract light to be focused on the retina. Any lesions of the lens will result in white discoloration and loss of transparency (cataract). This is seen as a white area in the central pupillary space. Young cataracts will appear as cloudy structures. A mature cataract appears as a completely white pupil.
A complete, mature cataract will reduce the vision of the elephant which may finally result in complete blindness of the affected eye. When an elephant is approached on the side of the blind eye, the clinician should be aware of the compensating behavior of the elephant, when it tries to keep its functional eye on the investigator.
Cataracts are quite common in Asian elephants in range countries. One paper notes that 6-8% of the elephants kept in Sri Lanka suffer from this condition (Kuruwita, 1991).
Several causes of cataracts are known in other animal species: trauma, overexposure to sun light, deficiency of vitamin A, C, E or riboflavin, diabetes and dehydration. Often the cause of a cataract in elephants cannot be determined.
Early stage of a cataract in an Asian elephant. (Photo: KUMar)


Advanced stage of a cataract in an Asian elephant. (Photo: KUMar)
Advanced stage of a cataract in an Asian elephant. (Photo: KUMar)

Panopthalmitis and phthisis bulbi
Panophthalmitis is inflammation of all layers of the eye including the intraocular structures. It has been documented in nine eyes postmortem during a field study of eye lesions in African elephants (McCullagh, 1969).
Phthisis bulbi is a shrunken, non-functional eye. It may result from severe eye disease, inflammation or injury.

Phthisis bulbi after chronically infected cornea ulcer. (Photo: KUMar)

Subdermal injection of Plancentrex (0.1 mg/ml) in an Asian elephant with uveitis. (Photo: KUMar)
Summary of the most frequently used drugs in ophthalmology


Standard frequency of treatment applications: 3-5 per day
Antibiotic treatment should be based on sensitivity test
Flushing with 0.9% NaCl solution is recommended before every topical drug application


The elephant's eye can be flushed using a long, small diameter tube place on a syringe. (Photo: KUMar)
Treatment options in elephant ophthalmology
Blepharitis: Treatments of blepharitis in elephants have not been described in the literature. A similar approach as in other mammals is recommended: elimination of the cause (parasites, dermatitis) and flushing the eye (see photo below) with saline solution, 3-5 times a day.
Conjunctivitis, prolapse of the conjunctival sac: elimination of the cause and flushing the eye with saline solution, 3-5 times a day and antibiotic ointment, 3-5 times a day.
Corneal edema: flushing with a hypertonic saline solution, 3-5 times a day.
Keratitis in early stage: flushing with saline solution, 3-5 times a day, antibiotic ointment, 3-5 times a day. If there is no ulceration, topical application of 0.1% dexamethasone eye drops may be used; be aware that corticosteroids will stop the regeneration of the epithelial cells.
Chronic keratitis: treatment will have no effect.
Xerophthalmia: oral vitamin A supplementation.
Corneal ulcer: flushing with saline solution, and topical application of antibiotic eye ointment 3-5 times a day. Topical application of Diclofenac sodium 1% eye solution may help reducing the pain. Promising results of the use of autologous serum have been reported (Janyamethakul, 2015), applied twice daily. Preparation of autologous serum: Five 10 ml. syringes were used to collect a total of 50 ml. Then, the blood was allowed to clot for 2 hours at room temperature before being centrifuged at 3,000 rpm for 15 minutes. The separated serum was collected (about 20-25 ml.) into a sterile container to which 1 mg. of gentamicin was added. The autologous serum was then aliquoted into sterile tubes, each containing 3 ml. Additionally, the serum was stored at 4°C and used within 7 days.
Topical treatment with acetylcysteine (0.02%) was used in case of a corneal abscess along with gentamycin and atropine (Pipitwanichtham, 2023).
Other treatments attempts that have been tried:
Indolent (non-healing) corneal ulcers are hard to treat. Debridement of necrotic corneal stroma should be considered. This can be done by using a cotton tip, or in more severe cases the abnormal cornea tissue can be scraped using a corneal spatula. Theoretically, after the debridement, the cornea should be protected by a contact lens as used in horses. This has been reported once in a 44 yrs-old Asian elephant, in which case the lens was lost soon after application. In elephants flushing the eye and applying antibiotic eye ointment and autologous serum is probably the only possible post-debridement treatment.
Stem cell application: promising results were seen at the Elephant Conservation Center Lampang (Thailand).
Although never reported in elephants, the application of a few droplets of cyano-acrylate might be an alternative for a contact lens in elephants.
Hypopyon: pain relief (NSAID), systemic antibiotics (DDX: leptospirosis!).
Uveitis and Synechia: Atropine sulfate eye ointment (1%), 4-6 times a day, is a commonly used mydriatic drug in horses. It may stabilize the blood-aqueous barrier, reducing vascular protein leakage, minimizing pain from ciliary muscle spasm, and reducing the chance of synechia formation by causing pupillary dilatation. Pupil dilation is an indicator for the drug to be effective on the ciliary muscles. In horses even topical atropine has been shown to prolong intestinal transit time, reduce and abolish intestinal sounds, and diminish the normal myoelectric patterns in the small intestine and large colon of horses. Whether this also applies to elephants is unknown. Subdermal injection of placental extract (Placentrex®) is a common treatment for uveitis, hypopyon and corneal opacities in elephants in Asia (Suedmeyer, 2006). See also photo below.
Iris prolapse: systemic NSAID, flushing with saline solution, 3-5 times a day. As the cornea is perforated by the prolapsed iris, the elephant should be treated systemically with antibiotics.
Cataract: only 2 cases of (mature) cataract removal by phaecoemulsification have been reported (cataract surgery-UK and cataract surgery-USA). However, artificial lenses to replace the removed lens contents are not available. The significant lens instability (first noted following the initial stages of surgery in the USA-case, i.e., during creation of the anterior capsulorhexis) prevented implantation of an intraocular lens implant. See for more detailed information the references below (Cerrata, 2019 and Manchip 2020).
Panophthalmitis: Enucleation is the only treatment indicated for this condition. However, there are no published data on the treatment of panophthalmitis.
References and further reading:
-
Bapodra P, Bouts T, Mahoney P, Turner S, Silva-Fletcher A, and Waters M. 2010. Ultrasonographic examination of the Asian elephant (Elephas maximus) eye. Journal of Zoo and Wildlife Medicine , Vol. 41, No. 3, 409–417.
-
Cerreta, A.J., McMullen Jr R.J., Scott, H.E., Ringenberg, J.R., Hempstead, J.E., DeVoe, R.S., Loomis, M.R., and Minter, L.J.. 2020. Bilateral Phacoemulsification in an African Elephant (Loxodonta africana). Hindawi Case Reports in Veterinary Medicine Volume 2019, Article ID 2506263, https://doi.org/10.1155/2019/2506263 or click here to download the manuscript.
-
Dangolla A, JS Edirisinghe and ID Silva (2005). Association of Acanthamoeba with a corneal ulcer in a captive elephant (Elephas maximum maximus). Proceedings of 57th Annual Convention and Scientific Sessions of the Sri Lanka Veterinary Association. 33pp
-
Fowler M. 2006. Infectious diseases. In: Biology, Medicine and Surgery of Elephants, Ed. Fowler and Mikota, 148.
-
Janyamethakul T, Moleechat P, Gohain R, Somgird C, Pongsopavijit P, and Wititkornkul B. 2015. Efficacy of Autologous Serum as An Adjunct Treatment for A Melting Corneal Ulcer in A Captive Asian Elephant. Thai Journal of Veterinary Medicine: Vol. 45: 2, Article 18.
-
Kraiwong, N., P. Sanyathitiseree, K. Boonprasert, P. Diskul, P. Charoenphan, W. Pintawong and A. Thayananuphat (2016). "Anterior ocular abnormalities of captive Asian elephants (Elephas maximus indicus) in Thailand." Vet Ophthalmol 19(4): 269-274.
-
Kuruwita VY and Abeysinghe AB. 1991. Surgical correction of blindness due to mature cataract in a domesticated Asian elephant. International Seminar on Veterinary Medicine in Wild & Captive Animals, Bangalore, India, November 8 to 10, 1991; 23
-
Manchip, K.E.L., Sayers, G., Lewis, J.C.M., and Carter, J.W. 2019. Unilateral phacoemulsification in a captive African elephant (Loxodonta africana). Open Veterinary Journal, (2019), Vol. 9(4): 294–300. ISSN: 2218-6050 (Online) DOI: http://dx.doi.org/10.4314/ovj.v9i4.3. or click here to download the manuscript.
-
Pipitwanichtham S, Dittawong P, Meetipkit P, Sitdhibutr R, Pattanapon N, Kasornsri M, Phetudomsinsuk K, Thongtip N, Sripiboon S. Case report: Corneal stromal abscess in a captive Asian elephant: diagnosis and treatment regimes. Veterinary Integrative Sciences 2023; 21(3): 693 - 703 DOI; 10.12982/VIS.2023.050.
-
Suedmeyer Wm. K. 2006. Special senses. In: Biology, Medicine and Surgery of Elephants, Ed. Fowler and Mikota, 399-403.
-
Wijesekara PNK, Bandara KAPA, Dangolla A, Silva ID and Edirisinghe JS. 2007. Incidence of Acanthamoebae Spp. in the eyes of a group of captive elephants in Sri Lanka. Conference: International Elephant Conservation & Research Symposium Florida USA At: Orlando, Florida USA, November 2007.
-
Wong MA, Isaza R, Cuthbert JK, Brooks DE and Samuelson DA. 2012. Periocular anterior adnexal anatomy and clinical adnexal examinaton of the adult Asian elephant (Elephas maximus). Journal of Zoo and Wildlife Medicine , Vol. 43, No. 4, pp. 793-80.
